Now Reading: Healthcare Dashboard Examples (Improving Patient Care)
-
01
Healthcare Dashboard Examples (Improving Patient Care)
Healthcare Dashboard Examples (Improving Patient Care)
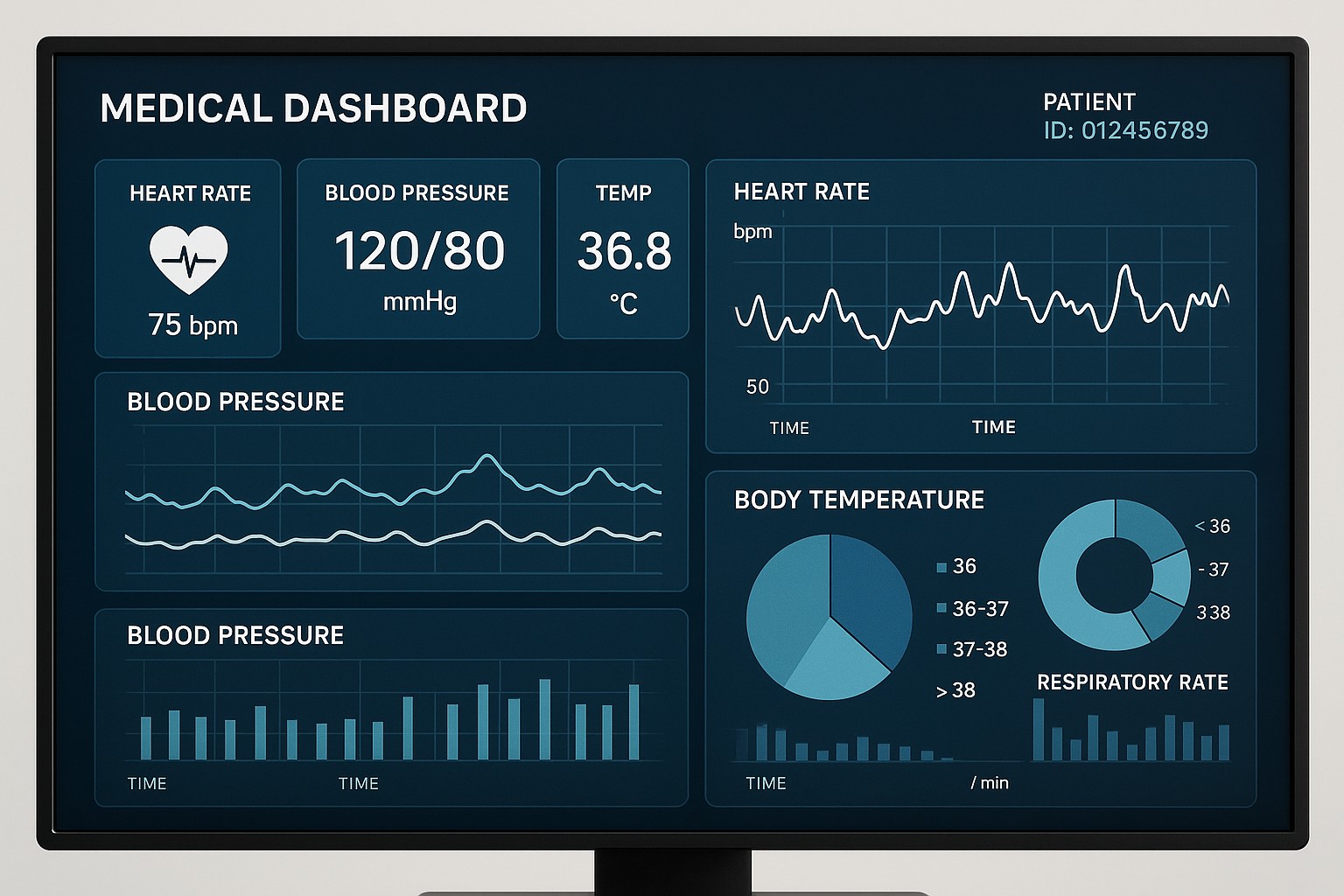
The Role of Healthcare Dashboards in Patient Outcomes
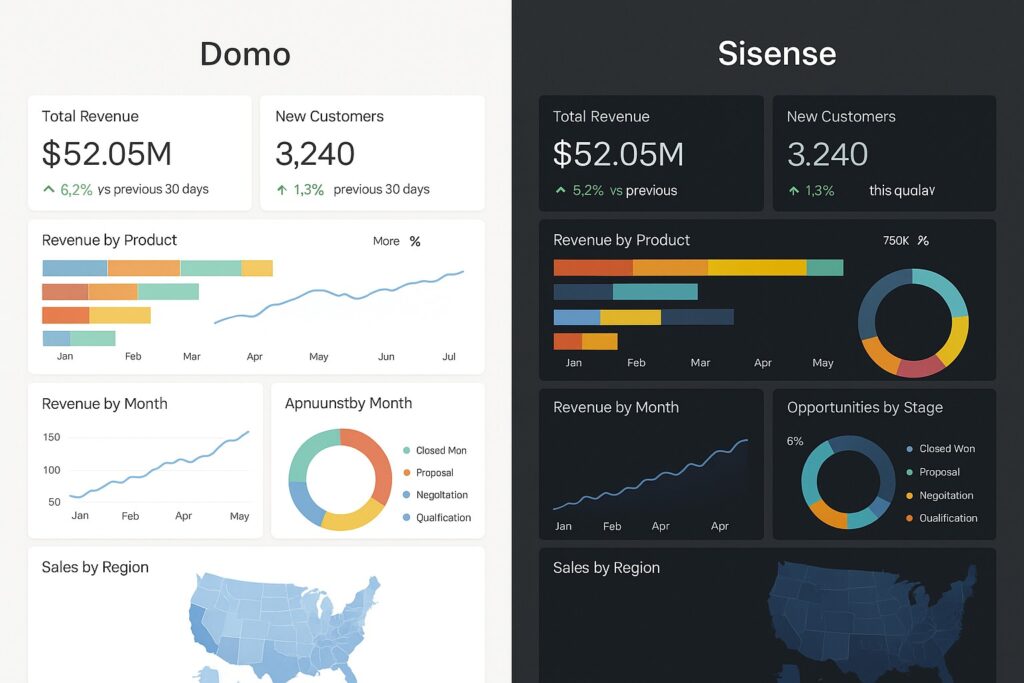
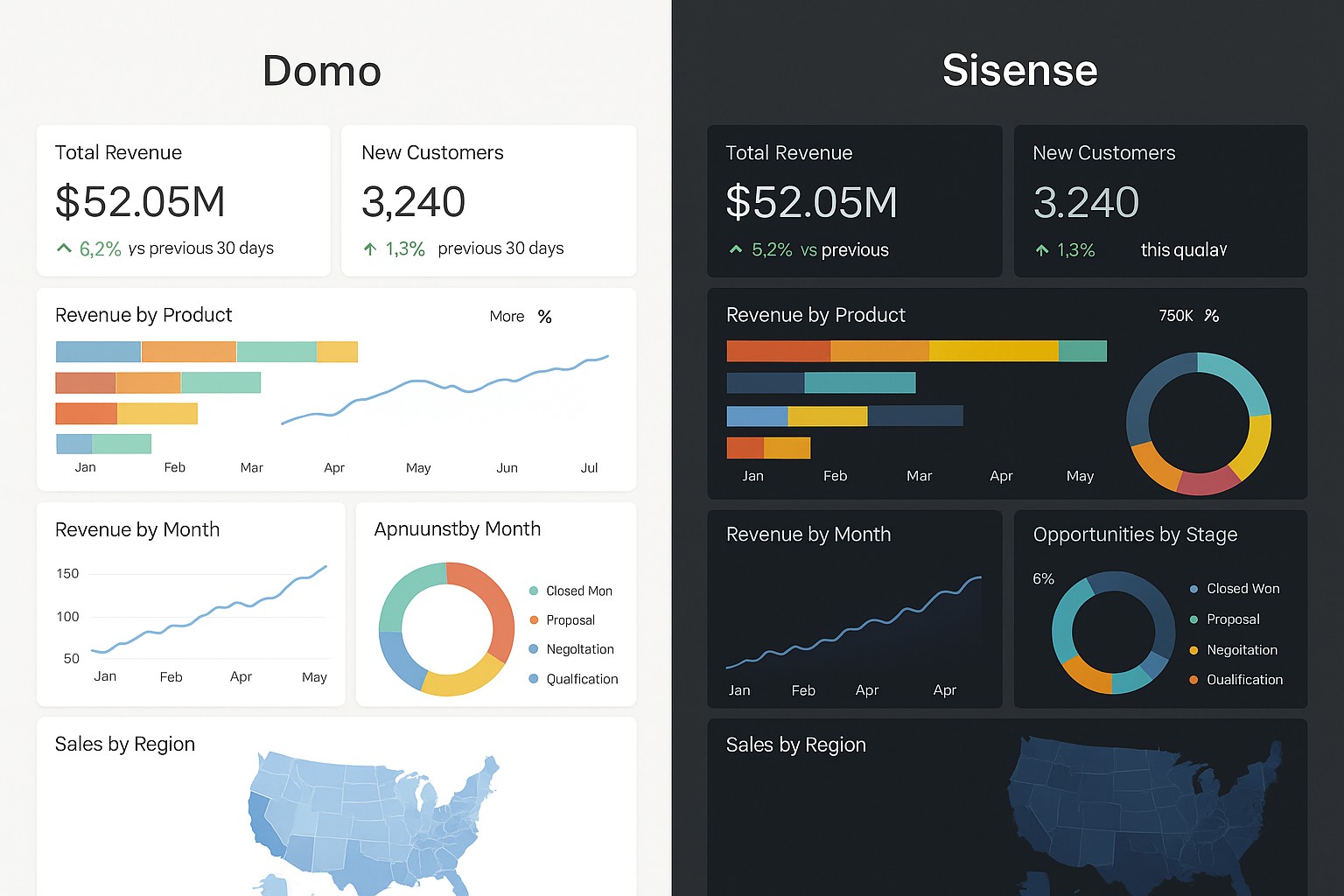
Healthcare dashboards enable organizations to synthesize data from electronic health records, laboratory information systems, imaging repositories, patient-reported outcomes, and administrative data into a single, coherent view. When thoughtfully designed, these dashboards surface trends in patient outcomes, risk factors, and clinical performance, helping clinicians and leaders understand where care is succeeding and where it needs improvement. They support proactive care by turning disparate data into contextual insights that inform daily decisions and strategic planning.
In clinical settings, dashboards act as a common operating picture that aligns multiple disciplines around shared goals. They empower physicians, nurses, case managers, and executives to monitor performance, identify bottlenecks, and execute rapid improvement cycles. The most effective dashboards balance depth with clarity, presenting high-level indicators on a single screen while permitting drill-down into lineage, context, and causality as needed. By providing near real-time visibility, dashboards help teams move from reactive firefighting to data-driven continuous improvement.
- Real-time visibility into clinical and operational performance
- Early warning signals for adverse events or deterioration
- Benchmarking across departments, units, and time periods
- Data quality assurance with lineage and provenance
- Actionable workflows and drill-down analytics for care coordination
Operational Excellence: Monitoring Throughput and Resource Utilization
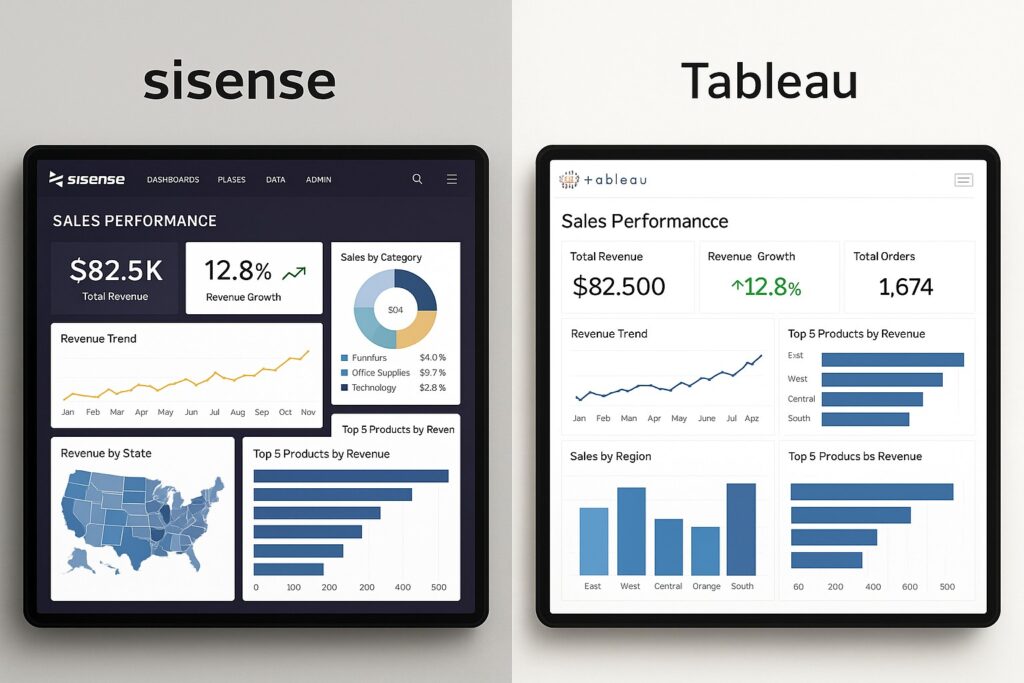
Operational dashboards translate patient flow, staffing, equipment availability, and supply chain data into actionable insights. They help hospital leaders anticipate capacity challenges, allocate resources efficiently, and optimize the care pathway from admission to discharge. By correlating bed status with staffing levels, patient acuity, and procedure schedules, these dashboards illuminate where process redesign or scheduling changes can yield faster throughput and improved patient experiences.
Below is a compact example of typical operational metrics, showing the intent behind each measure and common data sources that support them. The table illustrates how a hospital might monitor capacity and flow in a real-world setting.
| Metric | Purpose | Data Source | Typical Impact |
|---|---|---|---|
| Average Length of Stay (ALOS) | Assess efficiency and care pathways | EHR, admission/discharge data | Drives staffing and bed planning |
| Bed Occupancy Rate | Visualize capacity pressure | Bed management system, EHR | Improved patient flow |
| Readmission Rate (30 days) | Quality of care follow-up | EHR, claims data | Targets for discharge planning |
| Throughput by Unit | Identify bottlenecks in clinical units | Workflow and patient tracking systems | Optimized staffing and process changes |
Quality of Care Metrics and Compliance Tracking
Quality of care dashboards focus on patient safety, clinical effectiveness, and compliance with regulatory and accreditation standards. They integrate data from infection control, medication safety, adverse events, patient experience, and outcome measures such as mortality and complication rates. By aligning these metrics with internal targets and external benchmarks (for example, CMS quality measures or Joint Commission standards), organizations can quantify progress and direct improvement efforts where they matter most.
Dashboards for quality and compliance enable accountability without sacrificing clinician autonomy. They support rapid detection of deviations from targets, trigger root-cause analyses, and guide standardization of best practices across departments. When used properly, these dashboards facilitate transparent reporting to leadership, quality committees, and regulatory bodies while preserving clinician trust by presenting clear, context-rich information rather than overwhelming data dumps.
Data Governance and Security in Healthcare Dashboards
In healthcare, data governance and security are non-negotiable foundations for dashboard programs. Effective governance defines ownership, responsibilities, data quality standards, and interoperability rules so that dashboards rely on trusted, consistent data. Security considerations include protecting patient privacy, enforcing least-privilege access, and maintaining auditable trails for compliance with HIPAA and other regulations. A governance framework supports sustainable analytics, reduces risk, and fosters confidence among clinicians who rely on dashboards in patient care.
- Define data ownership and stewardship roles for each data domain (clinical, financial, operational).
- Implement role-based access controls and need-to-know access for PHI, with audit trails.
- Establish data lineage and provenance to trace data from source to dashboard.
- Apply data quality checks, standardized definitions, and normalization to support reliable analytics.
- Prepare incident response, downtime procedures, and regular audit reviews to maintain trust.
Designing Dashboards for Clinician Adoption and Usability
Designing for clinicians requires a human-centered approach that respects workflow, minimizes cognitive load, and prioritizes clarity over clutter. Effective dashboards present relevant information in a concise, scannable format, with visuals that encode critical signals (such as red/yellow/green status) and intuitive navigation for deeper exploration. Consistency in layout, terminology, and color schemes helps users form quick mental models, reducing time-to-insight during busy shifts.
Key design considerations include role-based views, standardized metrics, actionable alerts, and governance for version control and updates. Dashboards should enable rapid triage and decision support without replacing clinical judgment. A well-designed interface also supports mobility and offline access when needed, ensuring that clinicians can engage with the data where and when it matters most. “A dashboard should be a signal, not a data dump,” as many health analytics leaders remind teams to keep the surface clean and purposeful.
“A dashboard should be a signal, not a data dump.”
Implementation Roadmap and Change Management
Successful deployment of healthcare dashboards requires alignment across clinical leadership, information technology, analytics, and data governance. A practical approach begins with a clear problem statement, measured success criteria, and a data inventory that identifies source systems, data quality issues, and integration challenges. Early wins in a pilot unit can build momentum and demonstrate value before scaling to the enterprise.
A phased implementation typically includes discovery and data modeling, rapid prototyping with clinician feedback, a controlled pilot, and broad rollout with ongoing training and governance. Change management should address culture, incentives, and workflows to ensure adoption, along with robust monitoring to detect misuse, data drift, or unmet training needs. The result is a scalable, trustworthy dashboard program that continuously improves care delivery and operational performance.
What is a healthcare dashboard?
A healthcare dashboard is a visual interface that aggregates clinical, operational, and financial data from multiple systems to present key indicators and trends in a single view. It supports decision-making by enabling quick interpretation, drill-down analysis, and monitoring of performance against targets, all while maintaining data governance and security.
How do dashboards improve patient outcomes?
Dashboards improve patient outcomes by surfacing real-time or near-real-time insights that help clinicians detect deterioration earlier, adhere to evidence-based pathways, and coordinate care across teams. By tracking outcomes, readmissions, and process measures, dashboards guide targeted improvements that translate into safer, more effective care and better patient experiences.
What data sources do healthcare dashboards integrate?
Dashboards commonly integrate electronic health records, laboratory data, radiology and imaging systems, pharmacy feeds, scheduling and occupancy data, billing and claims information, patient experience surveys, and, increasingly, wearable device and remote monitoring streams. Interoperability standards such as HL7, FHIR, and DICOM enable these sources to be stitched together into a coherent analytics view while supporting governance and security requirements.
How is data security ensured in healthcare dashboards?
Security is addressed through access controls based on user roles, encryption at rest and in transit, strong authentication, and comprehensive audit logging. Data governance policies define data ownership, data quality, and data retention, while incident response procedures prepare teams to detect, contain, and remediate any breaches or downtime. Regular training and governance reviews help maintain a culture of security and compliance.
How should hospitals measure the ROI of dashboards?
ROI can be measured through a combination of time-to-decision improvements, reductions in length of stay and readmission rates, enhanced patient satisfaction, and cost savings from more efficient staffing, supply utilization, and workflow optimization. Tracking these metrics before and after dashboard implementation, while controlling for confounding factors, provides a credible view of value and guides ongoing investment and refinement.