Now Reading: Predictive Analytics in Healthcare: Transforming Patient Care
-
01
Predictive Analytics in Healthcare: Transforming Patient Care
Predictive Analytics in Healthcare: Transforming Patient Care

Strategic Value of Predictive Analytics in Healthcare
Predictive analytics in healthcare is increasingly framed as a strategic capability that aligns clinical excellence with operational efficiency. By transforming historical and real-time data into forward-looking insights, health systems can identify patients at elevated risk, anticipate resource shortages, and tailor interventions to achieve better outcomes at lower total cost of care. For executive teams, the value lies not only in improved patient safety and satisfaction but also in measurable gains in readmission reduction, bed occupancy optimization, and evidence-based prioritization of high-impact initiatives. As payer strategies shift toward value-based care, predictive analytics becomes a differentiator that enables proactive care management, precise population health strategies, and transparent performance reporting that stakeholders can trust.
Realizing this value requires a governance-aware approach that bridges clinical expertise with data science, IT infrastructure, and risk management. Organizations must invest in data quality, interoperability, and scalable analytics platforms while cultivating clinician champions who translate model outputs into actionable workflows. The most successful programs operationalize analytics through iterative pilot programs, formalized governance, and continuous monitoring. This ensures that models stay aligned with patient safety standards, regulatory requirements, and organizational goals, even as clinical guidelines evolve and patient demographics shift. In short, predictive analytics is not a one-and-done initiative but a continuous capability that supports decision-making across the care continuum.
- Improved readmission risk stratification and targeted care planning
- Optimized clinical pathways that shorten stay and reduce variability
- Early detection of infectious disease trends to inform public health and hospital readiness
- Efficient resource allocation, including staffing, bed management, and supply planning
- Ongoing monitoring of treatment outcomes to refine protocols and reduce practice variation
Key Models and Data Sources
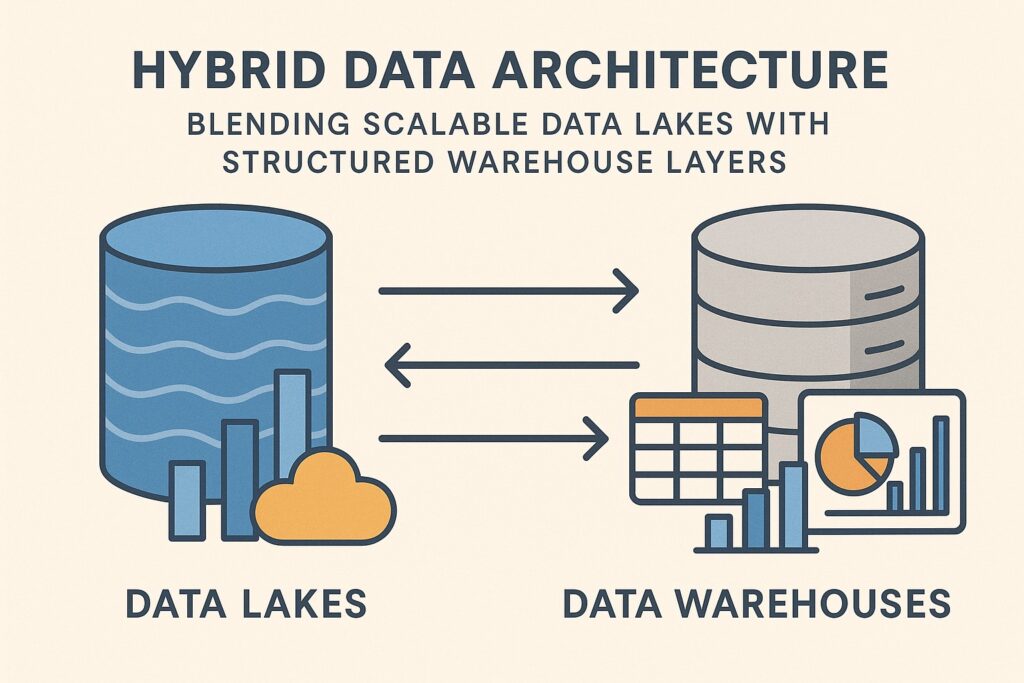
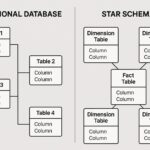
At the core of predictive analytics are models that can learn patterns from diverse data types, ranging from structured electronic health records to unstructured clinical notes, imaging, and sensor data. Common modeling approaches include logistic regression for interpretable risk scores, time-to-event (survival) models for event prediction over time, and ensemble methods such as gradient boosting and random forests that capture nonlinear relationships. More advanced techniques, including recurrent neural networks and transformer-based models, are increasingly used to extract insights from longitudinal data and free-text notes. Regardless of the method, models must be calibrated on representative data, validated across multiple sites, and exposed with appropriate explanations to support clinician trust and patient safety.
Data sources in healthcare analytics are broad and heterogeneous. They span inpatient and outpatient encounters, medication histories, laboratory results, imaging reports, wearable and home monitoring data, social determinants of health, and administrative claims. Unstructured data, particularly clinical narratives, often holds rich information about symptoms, functional status, and social context that structured fields miss. Effectively integrating these sources requires robust data governance, standardized vocabularies (such as SNOMED CT and LOINC), and privacy-preserving techniques. Quality control steps—data lineage, completeness checks, and bias assessments—are essential to ensure that model outputs reflect real-world conditions rather than artifacts of data collection or implementation context.
- Risk scoring models that predict adverse events, readmissions, or deterioration within defined time windows
- Outcome prediction models focused on treatment efficacy, long-term survival, or quality-of-life measures
- Time-to-event analyses that forecast the probability of events such as hospital readmission or relapse over time
- Utilization and operational models that forecast demand for beds, staff, imaging, and laboratory capacity
- Clinical decision support integrations that translate model predictions into recommended actions
Implementation Framework: From Data to Decision
Effective deployment begins with a clear problem statement and success criteria that tie directly to clinical goals and financial impact. Teams should assemble cross-functional cohorts including clinicians, health economists, data engineers, privacy officers, and IT operations to map data flows, identify data quality gaps, and design pilot workflows that minimize disruption to care delivery. A well-scoped plan reduces deployment risk and accelerates time-to-value while preserving patient safety and regulatory compliance. Early simulations and backtesting in a secure environment provide insight into potential outcomes before a live rollout, helping to set realistic expectations for stakeholders and payers alike.
Once a model is validated, integration with clinical workflows is critical for sustainable impact. This includes embedding risk scores into the EHR with contextual explanations, establishing triggers for clinician alerts, and creating dashboards that highlight changes in patient status. Ongoing monitoring and governance are essential to catch data drift, model decay, or unintended consequences. A disciplined approach to model risk management—documenting assumptions, access controls, audit trails, and escalation paths—ensures accountability and maintains patient trust. Finally, adoption hinges on change management: training, feedback loops with clinicians, and demonstration of tangible improvements in care processes and outcomes.
- Define success metrics in clinical and operational terms before development begins
- Identify and harmonize data sources with clear data ownership and quality checks
- Prototype in a secure environment with synthetic or de-identified data where possible
- Deploy in phased pilots with rigorous monitoring, feedback, and governance
Data Governance, Privacy, and Ethical Considerations
Protecting patient privacy and ensuring compliant data use are foundational to any predictive analytics program. Organizations must align with regulatory requirements such as HIPAA and relevant state laws, enforce robust access controls, and implement de-identification or pseudonymization where appropriate. Data stewardship practices should clearly delineate who can access data, for what purposes, and under what conditions. Documentation of data lineage and model governance helps demonstrate accountability and transparency to patients, clinicians, and regulators.
Beyond privacy, ethical considerations demand attention to bias, fairness, and explainability. Models trained on biased data can perpetuate disparities in care. It is essential to conduct bias assessments across demographic groups, report performance gaps, and design safeguards that prevent automatic decisions from superseding clinician judgment. Explainability is equally important: clinicians need intuitive rationales for predictions, and health systems benefit from decision aids that present rationale, confidence levels, and alternatives. Engaging patient advocates and frontline clinicians in governance discussions fosters trust and ensures that analytics support, rather than overwhelm, clinical decision-making.
Case Studies: Readmission Management and Chronic Disease Prediction
In readmission management programs, predictive models identify patients at highest risk of hospital return within 30 days of discharge. By combining clinical indicators, social determinants, and previous care patterns, care teams can implement targeted interventions such as close post-discharge follow-up, medication reconciliation, and home health support. The impact is typically measured through reductions in 30-day readmission rates, shorter average length of stay for high-risk cohorts, and improved patient satisfaction. Critical success factors include seamless integration with discharge planning processes, timely data refreshes, and a closed-loop mechanism where outcomes inform ongoing model refinement.
Chronic disease prediction and management rely on longitudinal models that monitor disease trajectory, response to therapy, and adherence. By forecasting progression in conditions like diabetes, cardiovascular disease, or chronic kidney disease, providers can tailor preventive strategies, adjust treatment intensity, and allocate resources for high-need patients. The most effective programs align predictive insights with personalized care plans, enable proactive outreach, and integrate with patient engagement platforms to support behavior change. Across these cases, the common thread is a deliberate pairing of data-driven insight with clinician judgment and patient-centered care processes, yielding durable improvements in both health outcomes and system performance.
Future Trends: AI, Real-Time Analytics, and Operational Impact
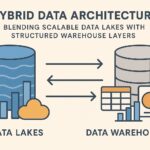
The next era of predictive healthcare analytics is defined by real-time data ingestion, richer sensor streams, and more sophisticated inference. Real-time analytics enable clinicians to detect deterioration as it happens, trigger timely interventions, and adjust care plans dynamically. Edge computing and secure streaming pipelines reduce latency and support decision-making at the point of care, while cloud-scale analytics unlock the capacity to model population-level risk alongside individual patient trajectories. As models become more capability-rich, health systems can move from retrospective insights to proactive, continuous optimization of care delivery.
Scaling predictive analytics across a health system requires interoperability, standardization, and robust governance. Open standards for data exchange, common evaluation metrics, and shared reference architectures help new sites replicate success. As adoption grows, executive dashboards and operational KPIs evolve to reflect both clinical outcomes and financial performance, including cost per attributable clinical improvement and return on analytics investments. The human element remains essential: clinicians and administrators must be equipped with the right tools, training, and organizational incentives to sustain a culture of data-informed decision-making.
FAQ
How does predictive analytics reduce readmission rates?
Predictive analytics reduces readmissions by early identification of patients at heightened risk of returning to the hospital and by enabling targeted, evidence-based interventions. Risk scores derived from clinical data, prior encounter history, and social determinants help care teams prioritize post-discharge follow-up, ensure medication reconciliation, schedule timely outpatient visits, and coordinate home health services. By aligning resources with those most in need and continuously monitoring outcomes, health systems can interrupt the trajectory toward a readmission, thereby lowering readmission rates and improving patient experience.
What data sources are essential for building reliable predictive models in healthcare?
Reliable models typically rely on a combination of structured data from electronic health records (diagnoses, procedures, labs, vitals), administrative data (billing codes, admission/discharge information), and unstructured data such as clinical notes. Supplementary sources include imaging reports, pharmacy data, wearable device feeds, and social determinants of health. The most robust models integrate multiple modalities, apply natural language processing to extract meaningful signals from text, and ensure data quality through rigorous governance, lineage tracking, and bias assessment.
How is patient privacy protected in predictive analytics projects?
Patient privacy is protected through a combination of de-identification or pseudonymization where feasible, strict access controls, encryption, and auditing. Data use is governed by formal agreements, and analytics work is often performed in secure environments with limited exposure to identifiable information. Organizations also implement privacy-by-design principles, minimize data collection to what is strictly necessary, and apply data minimization and retention policies aligned with regulatory requirements and organizational risk tolerance.
What are the biggest challenges in deploying predictive analytics into clinical workflows?
The most significant challenges include data quality and integration across disparate systems, clinician trust in model outputs, and the risk of alert fatigue or workflow disruption. Addressing these requires close collaboration with clinical teams, transparent model explanations, and careful integration into existing workflows with decision support that augments rather than replaces clinician judgment. Additional hurdles include maintaining governance and compliance as models evolve, ensuring equitable performance across patient subgroups, and securing sustainable funding for ongoing maintenance, monitoring, and improvement efforts.